Becoming Your Own Pain Management Expert
Goal
To be able to understand what it means to self-manage chronic pain and to gain self-awareness
Being a Pain Self-Manager (Turk & Winter, pp. 9-10)
People who are pain self-managers have gradually learned what they are capable of doing, and they have done that and gained even more capability. Although pain once held them completely in its grip, they have found ways to overcome its debilitating effects. While others can support you, you must become your own expert on your pain and your own pain manager. Nobody knows your pain as well as you do.
The Nature of Chronic Pain (Turk & Winter, pp. 10-14)
Pain following overuse or injury is considered to be chronic when it continues to interfere with living or does not become much less intense after the expected period of healing. Pain is also considered chronic when it is related to a progressive disease, such as arthritis or cancer. There are many common chronic pain conditions such as back pain, migraine and tension headaches, whiplash, and fibromyalgia. Chronic pain can be severe and cause significant distress and disability even when it has no clear physical cause. When this is the case, it is helpful to ask “What can I do to manage my pain so that I can get on with my life?” rather than “How or why did I get the pain?”.
Treatments for Pain (Turk & Winter, pp. 17-24)
There are numerous medical treatments for pain including the following:
 Analgesic medication
Analgesic medication- Antidepressants
- Mixed agent drugs
- Sedatives, tranquilizers, and muscle relaxants
- Anticonvulsants
- Topical agents
- Surgery
- Nerve blocks
- Trigger point injections
- Thermal therapies
- Electrical and ultrasound stimulation
- Chiropractic manipulations
- Acupuncture
- Biofeedback
- Pain clinics and rehabilitation programs
This course emphasizes self-managing chronic pain, which emphasizes:
 Pacing
Pacing- Gaining self-awareness
- Relaxing
- Changing thoughts and feelings
- Changing behavior
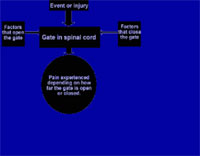
The Gate Control Theory (Turk & Winter, pp. 14-15)
Imagine a door or gate in your spinal cord. Before your pain became chronic or before you had a progressive disease, usually this gate was closed and you did not feel pain. If you had an injury or some other type of obvious physical damage occurred, signals were sent along your nerves to the spinal cord. These signals opened the gate and allowed information about the injury or damage to your body to reach the brain. This is where these signals are interpreted, with the result being the feeling of pain. In these cases, as you healed sometimes the pain was better and sometimes it was worse. It depended on how far open or closed the gate was. The following factors can open and close the pain gate:
| Factors | Open the Pain Gate | Close the Pain Gate |
|---|---|---|
| Physical Factors | Extent of injury | Medication |
| Counterstimulation (heat, rubbing) | ||
| Inappropriate activity level | Appropriate activity level | |
| Rest | ||
| Emotional Factors | Depression | Relaxation |
| Worry/fear | ||
| Tension | Positive emotions (happiness, optimism) | |
| Anger | ||
| Thoughts | Focusing on the pain | Life involvement, increased interest in life activities |
| Boredom due to minimal involvement in life activities | Concentration/distraction | |
| Non-adaptive attitudes and expectations (“It will never end!” “I’m helpless and hopeless!”) | Adaptive attitudes/positive thoughts and feelings (“I can control my feelings.” “I can reduce my level of muscle tension.” “I am capable of doing many things despite my pain.”) |
Pain Rating & Functional Pain History Exercise (Turk & Winter, pp. 27-28)
Instructions: Documenting and rating your pain is critical. Doing so results in putting on paper a beginning knowledge of your pain that you can build on as you complete this course.
In considering the following ratings, think of each one on a continuum. For example, with regard to rating pain, (0) means that you do not feel even a hint of discomfort. Very intense pain (6) means that you can barely move without feeling you may pass out from the pain. In the middle (2-5), you are aware of varying degrees of pain. As another example, if you were rating “days,” when you are experiencing a (1) level, you are having a really “good” day. When you are experiencing a (6) level, you are likely having a really “bad” day. In the middle (2-5), you are having a kind of “middle good” or “middle bad” day.
| Pain Rating System | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Date Completed: _______________ | ||||||||||||||
|
1. Rate the level of your pain at the PRESENT MOMENT:
| ||||||||||||||
|
2. In general, during the PAST WEEK how much did your pain interfere with daily activities?
| ||||||||||||||
|
3. During the PAST WEEK, how much has your pain changed the amount of satisfaction or enjoyment you get from taking part in social and recreational activities?
| ||||||||||||||
|
4. On average, how severe has your pain been during the PAST WEEK?
| ||||||||||||||
|
5. During the PAST WEEK, how irritable have you been?
| ||||||||||||||
|
6. During the PAST WEEK, how tense or discoursed have you felt as a result of your pain?
| ||||||||||||||
Complete this table:
| Functional Pain History |
|---|
| Date Completed: _______________ |
|
A. Below is a list of activities. Circle the letter of any one that you feel you can no longer do because of your pain.
a)Cook meals
b)Work on the car c)Go to the movies d)Work in the garden e)Visit with friends f)Go hunting or fishing g)Play cards or board games h)Go to a place of worship i)Go to/shop at the mall
j)Play sports (golf, tennis, etc)
k)Clean the house l)Work on hobbies m)Walk in the park n)Hold a job o)Other _________________ p)Other _________________ q)Other _________________ |
|
B. Make a list of the things you CAN do despite your pain (e.g., talk on the phone, watch TV, read a magazine).
_________________________
_________________________ _________________________ _________________________ _________________________ _________________________
_________________________
_________________________ _________________________ _________________________ _________________________ _________________________ |
|
C. Circle the letter of the things that have made your pain worse in the past.
a)Weather
b)Exercise c)Stress d)Cold e)Heat
f)Arguments
g)Fatigue h)Poor sleep i)Depression j)Other (describe)_________________________ |
|
D. Circle the letter of the things that have made your pain better in the past.
a)Rest
b)Warm bath c)Relaxation d)Sleep e)Medication
f)Exercise
g)Other (describe)_________________________ h)Other (describe)_________________________ i)Other (describe)_________________________ |
Next Step
Learn more about The Gate Control Theory by watching the following video:
 Analgesic medication
Analgesic medication Pacing
Pacing